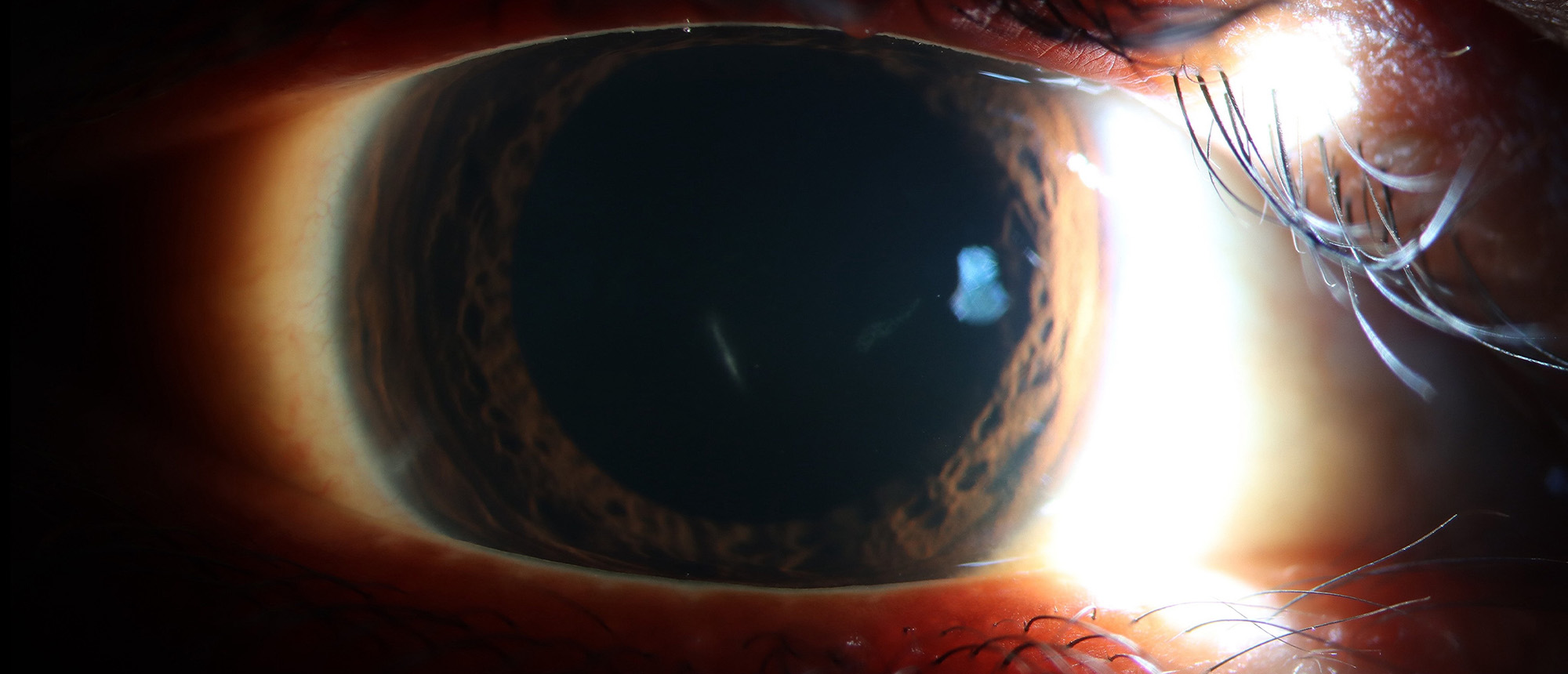
Suspected Early Traumatic Exogenous Endophthalmitis
A patient presented to the Bascom Palmer Eye Institute Emergency Room after a palm frond struck his right eye while working. Initial evaluation revealed visual acuity of 20/30 with pinhole correction to 20/25 in the affected eye, 2-3+ anterior chamber cell and flare with inferior endopigment dusting, and a linear 1×1mm corneal laceration extending to 90% depth from inferonasal to superonasal, Seidel negative with pressure. Anterior segment OCT confirmed near-full thickness laceration with intact Descemet's membrane. Dilated fundus exam was unremarkable bilaterally. Despite an initially reassuring exam, the patient's clinical picture — particularly the anterior chamber inflammation, organic mechanism of injury, and depth of the corneal wound — prompted empiric broad-spectrum intravitreal antibiotic and antifungal prophylaxis. The patient was managed with intravitreal vancomycin and ceftazidime and voriconazole with close surveillance and ultimately achieved visual stabilization. This case highlights the diagnostic challenge of post-traumatic endophthalmitis in the setting of a Seidel-negative wound, the unique polymicrobial inoculation risk of organic and plant-matter ocular trauma, and the importance of empiric broad-spectrum coverage — including antifungal prophylaxis — when vegetative injury is the mechanism. It further underscores the epidemiological relevance of palm frond and gardening injuries in tropical and subtropical regions such as South Florida, where such occupational hazards are endemic.
Presentation Date: 03/19/2026
Issue Date: 03/27/2026
Please log in or click on ENROLL ME to access this course.

