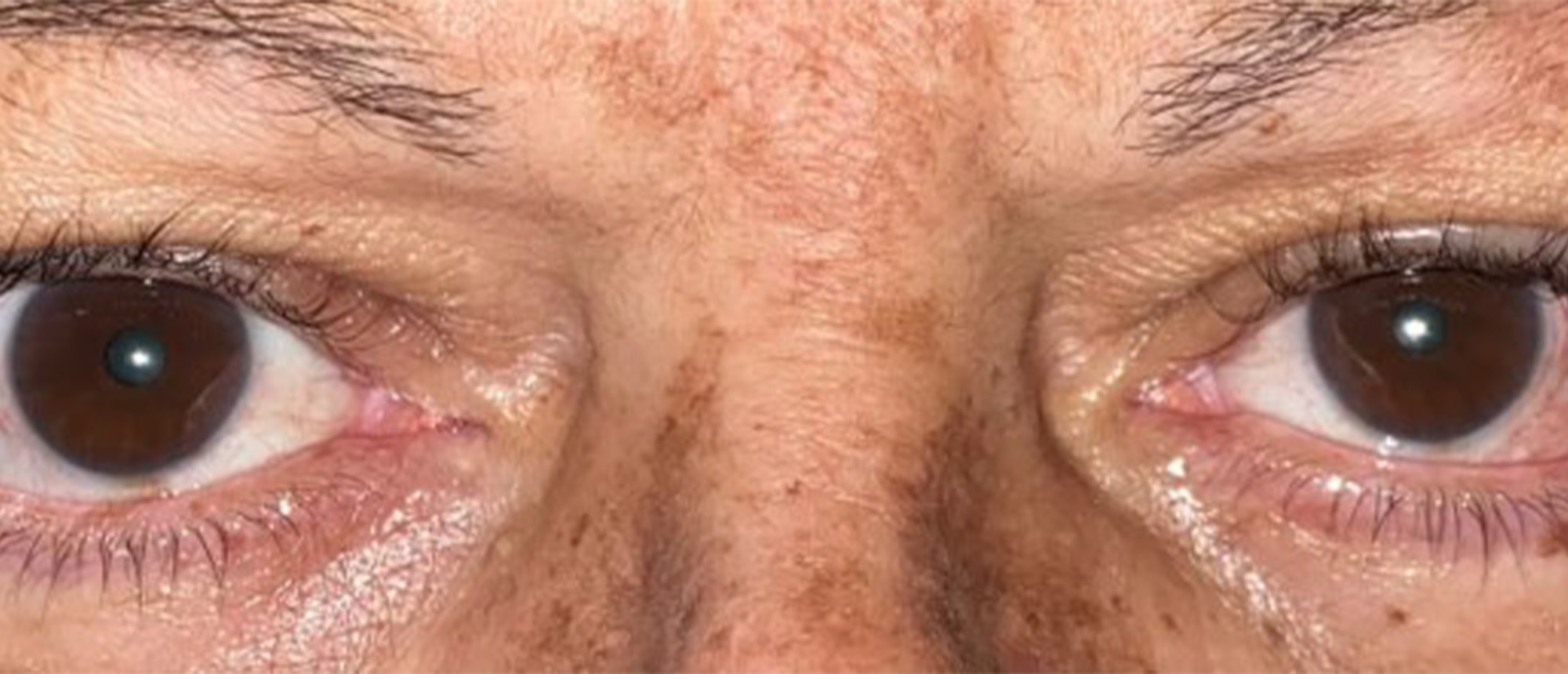
Partial Left VI Nerve Palsy
A patient with a history of recurrent optic neuritis and pontine telangiectasia presented with progressive binocular horizontal diplopia, worse at distance, associated with a compensatory face turn to the left causing neck pain. Best-corrected visual acuity was 20/20 in both eyes, with normal pupils and no relative afferent pupillary defect. Examination revealed a 30 prism diopter esotropia at distance in primary position, 15 prism diopters at near, a -3 to -4 abduction deficit of the left eye, a Y-pattern anisotropia, and normal stereopsis. A forced duction test demonstrated mild restriction in abduction, and the active force generation test showed moderate force at the forceps. Saccadic velocity was preserved. Maddox rod testing revealed no torsion. The patient was diagnosed with a left sixth cranial nerve palsy secondary to pontine telangiectasia. After neurology clearance confirming stable disease, surgical correction was performed using Mendonça's double interlacing technique on the left eye, in which the lateral rectus is split longitudinally and interlaced through the split superior and inferior rectus muscles without disinserting the vertical recti, thereby preserving anterior ciliary circulation. At post-operative day 9, the patient was orthotropic at both distance and near with no diplopia. At 6 months and 1 year follow-up, stable alignment was maintained (ET 1-4 PD at distance), with resolution of diplopia, improved abduction, and normal head posture.
Presentation Date: 03/05/2026
Issue Date: 03/27/2026
Please log in or click on ENROLL ME to access this course.

